Researchers discover new approach to treat allergic asthma
Washington, US: Researchers revealed that a protein known as Piezo1 stops allergens from hyperactivating a kind of immune cell in the lungs. The work implies that activating Piezo1 could be a new therapeutic approach to lowering lung inflammation and treating allergic asthma.
Type 2 innate lymphoid cells (also known as ILC2s) are immunological cells found in the lungs, skin, and other parts of the body. When allergens enter the lungs, ILC2s activate and create proinflammatory signals that drive the recruitment of other immune cells. Unchecked, this can lead to excessive inflammation.
Findings of the researchers from University of Southern California's Keck School of Medicine were published in journal of Experimental Medicine.
"Given the importance of ILC2s in allergic asthma, there is an urgent need to develop novel mechanism-based approaches to target these critical drivers of inflammation in the lungs," says Omid Akbari, Professor of Immunology and Professor of Medicine at USC's Keck School of Medicine.
Akbari and colleagues discovered that, when they are activated by an allergen, ILC2s start to produce a protein called Piezo1 that can limit their activity. Piezo1 forms channels in the outer membranes of cells that open in response to mechanical changes in the cell's environment, allowing calcium to enter the cell and change its activity.
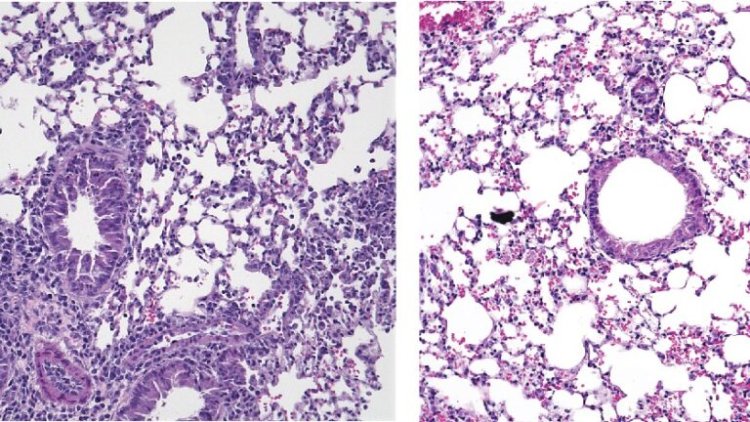
Akbari's team found that, in the absence of Piezo1, mouse ILC2s became more active than normal in response to allergenic signals, and the animals developed increased airway inflammation. In contrast, treatment with a drug called Yoda1 that switches on Piezo1 channels reduced the activity of ILC2s, decreased airway inflammation, and alleviated the symptoms of allergen-exposed mice. The group's observations suggest a significant role for Piezo1 channels in ILC2 metabolism, as treatment with Yoda1 reduced ILC2 mitochondrial function and rewired the cells' energy source.
Finally, the researchers determined that human ILC2s also produce Piezo1, and so they tested the effects of Yoda1 on mice whose ILC2s had been replaced with human immune cells.
"Remarkably, treatment of these humanized mice with Yoda1 reduced airway hyperreactivity and lung inflammation, suggesting that Yoda1 may be used as a therapeutic tool to modulate ILC2 function and alleviate the symptoms associated with ILC2-dependent airway inflammation in humans," Akbari says. "Future studies are therefore warranted to delineate the role of Piezo1 channels in human patients with asthma and develop Piezo1-driven therapeutics for the treatment of allergic asthma pathogenesis."















































